Last Updated on July 8, 2021
First of all, let’s watch a 3D animation video of how IVF works.This IVF Video is excellent for describing each and every process of In Vitro Fertilization.
Naturally, if you’re considering IVF, you’ve probably had several questions go through your mind. If you wonder about IVF procedures then continue reading.
Contents
Will IVF Work For You?
Before any In Vitro Fertilization (IVF) procedure is done, your fertility doctor or specialist is going to determine whether or not IVF is right for you. Several factors might rule out the possibility of becoming pregnant even with IVF. So expect to spend quite a bit of time evaluating whether or not IVF treatment is possible based on your circumstances.
If you’re very unlikely to become pregnant, your fertility doctor will recommend other treatment, or might success you go with a surrogate. To get to that conclusion, though, your doctor will consider many things.
From the start, you’ll go through what is typically called a Fertility Evaluation. Every clinic approaches a fertility evaluation differently but it consists of a psychological evaluation as well as a physical one. Physically, a fertility doctor looks for the likelihood of pregnancy by examining the uterus, the sperm, the ovaries, and eggs.
Fertility Evaluation and Assessments
One clinic based in Chicago, Conceptions, lists 5 questions that assessments are trying to answer. Depending on the results from these tests or questions, your doctor can more easily determine the likelihood of IVF procedures working for you.
“Does the woman produce and release an egg at regular intervals?”
You can take medications to regulate the production of eggs and you can also use this same medication to produce more eggs. So the point of this question isn’t merely to rule out IVF procedures, but really, to understand how much additional help you might need.
However, if the ovaries don’t produce any eggs at all, IVF using fresh, non-donor eggs isn’t possible. You can still do IVF with donor eggs, though, as long as other hurdles are cleared.
“Does the man produce adequate numbers of healthy sperm?”
IVF require healthy, motile sperm. Again, not having healthy sperm, or having too little sperm, doesn’t rule out IVF procedures. You can use donor sperm. Or, if you’d prefer, you can take medications or treatments to increase the volume and motility of sperm.
“Can the egg and sperm unite in the woman’s reproductive tract?”
If so, then you might not need IVF at all – or, it could be that IVF isn’t going to help your specific fertility issue. In vitro fertilization assists in the fertilization of egg and sperm. If the fertility issue isn’t due to that, and is due to something like implantation or uterine lining problems, IVF procedures might not be of great assistance. Knowing this helps fertility doctors provide realistic odds of their IVF treatment resulting in a live birth.
Additional questions include “Do the sperm and egg combine to form a fertilized egg and divide to form an embryo?” and “Is the embryo able to implant and thrive in the uterus?”
IVF Statistics – Which rates matter?
Before starting IVF procedures, your fertility clinic’s doctor or nurse will share success rates. There are two types of success rates: pregnancy rates and live birth rates.
Pregnancy rates tell you the ratio of embryo transfers resulting in pregnancy to those that didn’t. Live birth rates, on the other hand, tell you the ratio of embryo transfers resulting in live births, and those that didn’t.
There is some debate about which statistics matter the most. Ultimately, both rates provide valuable information. The reason you should ask about live birth rates, primarily, is that many pregnancies subsequently terminate (naturally) and therefore only a percentage of women who become pregnant through IVF will go on to have a baby. While the reasons for a pregnancy ending shouldn’t be directly tied to the IVF clinic, it’s good information to know.
The IVF Treatment Process
Once you’ve passed a fertility evaluation and your fertility doctor has recommended IVF procedures, you’ll begin to prepare for IVF. The IVF process has six important parts. Your fertility clinic will oversee each of these procedures and processes and provide assistance and additional treatment as necessary.
Before You Start: Fertility Terms and Acronyms
Knowing the most common terms and acronyms that your fertility specialists and others use will help you prepare for treatment.
- OB/GYN: Obstetrician/Gynecologist. May initially diagnose your infertility and help plan for fertility treatment, but is likely not a fertility specialist or RE.
- RE: Reproductive Endocrinologist. RE’s specialize in certain disorders, including endometriosis.
- IUI: Intrauterine insemination. Involves placing sperm inside the uterus.
- ICSI: Intracytoplasmic Sperm Injection. Involves injecting sperm directly into an egg (rather than mixing sperm and egg together in a dish).
- hCG: Human chorionic gonadotropin (otherwise known as the pregnancy hormone).
- FSH: Follicle stimulating hormone. As the name implies, FSH stimulates the ovaries to rapidly mature follicles.
- FET: Frozen embryo transfer.
- TWW: Two week wait. Commonly used by women and men going through IVF procedures. Describes the two week waiting period after embryo transfer.
- TTC: Also commonly used by those going through IVF. It stands for trying to conceive.
1. Preparing for IVF
Your fertility clinic will prepare you for IVF procedures by meeting with you, discussing and prescribing medications, talking about your cycle, and planning things out. Not all IVF cycles are the same. Even the medications given to patients prior to starting an IVF cycle can be different, because all bodies and circumstances are unique.
Most patients are given medications to suppress their own natural menstrual cycle, and that’s because the start of a menstrual cycle is the start of an IVF cycle, and it has to be regulated and planned for. IVF is a step-by-step process that relies heavily on timing. So your doctors and nurses will assist you with this process.
You’ll likely be given a medication called Lupron – or a similar medication – that you’ll inject yourself with. Lupron will suppress ovulation so that your doctor can monitor and retrieve the egg(s) later.
Some patients are also given birth control medication to get on a regular cycle, while taking Lupron toward the end of the cycle. According to one fertility treatment clinic, birth control pills benefit women who don’t have normal periods.
Some experts suggest that you begin “preparing” for IVF long before these parts of the process. According to some people, improving your diet, overall nutrition, and exercise can increase the success rate of IVF procedures by improving the quality of your egg(s). Other women have gotten rid of caffeine or sugar, or a variety of other things, in order to prepare for IVF.
2. Inducing Ovulation (7 to 14 days)
Normally, a woman’s ovaries produce one egg every month. But with IVF, many eggs are necessary, because not all eggs will become fertilized. Also, if you have a large number of eggs that do become fertilized embryos, you can freeze them for use later.
IVF procedures require ovulation of multiple eggs. You’ll given medication to make sure that happens. The most common medication is an injectible called Clomid. It’s also the cheapest. However, some fertility clinics don’t use Clomid, and use hormone medications called gonadotropins. There is some debate about which route is the best to use, but either way, the intended outcome is the same.
How ovulation induction works: Your doctor will prescribe a medication that you’ll take to stimulate the follicles in your ovaries. This works in two ways: you’ll produce more follicles (which in turn produce more eggs) and your follicles will mature more quickly. Follicles will not release eggs until they are mature, so the medication does that, too.
Ovulation induction in IVF looks very different than ovulation induction in intrauterine insemination (IUI). So, if you are doing a lot of research on your own make sure you are aware that the processes use the same names, but are different. In IVF procedures, your fertility doctor will always attempt to get to you to produce at least 10 eggs. In IUI, only one viable egg is actually necessary.
Vaginal Ultrasounds. Your doctor will use vaginal ultrasounds and other testing – including hormone testing – to monitor the progress of your ovaries, follicles, and eggs, so you may have several appointments or lengthy appointments during this process.
If the medication works and your body produces multiple eggs, they next step is to retrieve them.
3. Retrieving the Eggs and Sperm
At this point in the process, your ovaries should be functioning well and the follicles have matured, producing multiple eggs. Keep in mind that IVF procedures begin with suppressing ovulation, so your doctor will have to stimulate it.
In order to get the eggs ready to be retrieved, you’ll likely be given hcg, which is a medication that essentially tells the ovaries that it is time to ovulate. It does not take long – just 35-36 hours – so the timing is critical here.
You will likely be sedated during the egg retrieval process. Some fertility clinics actually induce sleep, while others just use a mild sedative. Either way, it’s unlikely that you will be alert during this procedure. To retrieve the eggs, your doctor will insert a small, hollow needle into the follicles, and then collect fluid – which hopefully contains eggs – through the needle.
Not all follicles produce eggs, and not all eggs that are produced are viables. This is a difficult and sometimes painful reality for people who are going through IVF. While fertility specialists hope that everything done up through this point results in healthy eggs, it’s impossible to know until they are collected.
Sperm is also collected at this time. If frozen sperm is being used, it will be thawed out, in order to be ready to fertilize the eggs.
After sperm and eggs are collected, you’ll be sent home with some recovery instructions and guidance for the next steps.
Read more: Understand egg retrieval process, preparation, and recovery
4. Fertilizing the Eggs – Same Day as Retrieval
The fertility clinic will count the eggs and also determine how many will be used for fertilization the same day they are retrieved. Only living, viable, mature eggs can be used.
In a fertility lab, a technician will mix the collected, healthy eggs with 50,000 to 100,000 sperm in order to fertilize at least one egg. Only one sperm will fertilize an egg, and it takes just a few hours for this to occur, usually.
Once the eggs are fertilized, the fertility clinic will allow 3 to 5 days for embryos to develop. When a fertilized egg begins to divide, it is called an embryo, and it takes approximately three days. As an embryo matures, it becomes a blastocyst. Typically, IVF procedures use embryos and do not need to wait until they become blastocysts. It will all depend on your specific situation, though.
Your clinic will communicate with you during this time. They will tell you if the eggs become fertilized, and how many, as well as if embryos begin to develop, and how many. If anything goes wrong during this process, you may be called in to talk about other options. Or, your doctor might request another sperm sample to continue fertilization.
If none of the eggs become fertilized, and there are no additional eggs to try, your doctor will likely discuss your options and may recommend another cycle of IVF treatment. Keep in mind that even completely unassisted pregnancy has a 15-20% chance of happening in any given cycle. If fertilization does not happen or if later stages of IVF fail, that doesn’t mean IVF will not work at all. It might just take more than one cycle.
If the embryos are healthy, growing, and ready, your clinic you’ll go in for an embryo transfer.
5. Transferring the Embryo (or Blastocyst)
For many couples, this is the most exciting day of the IVF treatment, while it’s also nerve-racking. At this time, one or more embryos will be inserted into the uterus, and the hope is that the embryos) will implant into the uterine lining and continue to divide and multiply.
This process is short, and every clinic does it a little differently. Be prepared for a serious discussion about how many embryos to transfer, and what to do with any that are not transferred. You have a few different options:
- Freezing. Fertility clinics can freeze developed embryos so that they can be used later on, either in subsequent IVF procedures, or donated to someone else.
- Discarding. Some patients choose to discard extra embryos. Your clinic will explain exactly how this process works.
- Transferring. You can transfer the developed embryos to the uterus. Again, this is a choice you, your fertility doctor, and potentially a specialist will make together.
Risk of multiples. If you choose to transfer more than one embryo, you may become pregnant with twins, triplets, or more. For some, it is a risk worth taking, but for others, the risk of multiples increasing the risk of a preterm baby or serious issues with the pregnancy. Talk to your doctor at length about this until you’re comfortable with your choice.
Blastocysts or Embryos. Some fertility clinics have higher pregnancy rates using blastocysts (matured embryos). Additionally, many clinics always transfer at least two embryos, and sometimes three. Transferring more embryos or blastocysts increases pregnancy rates but also increases the likelihood of multiples.
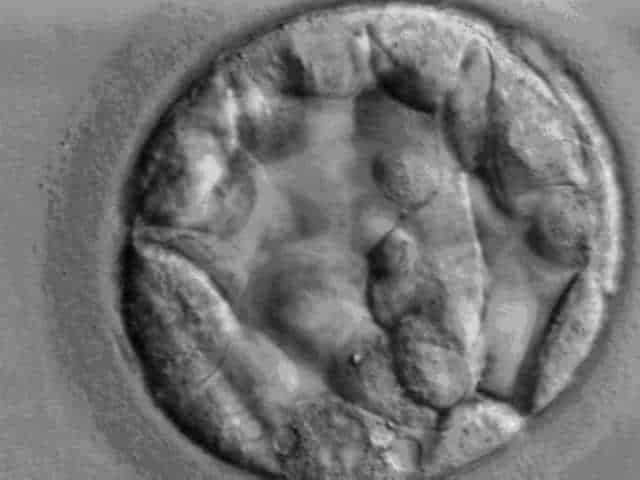
Image: Day 5 Blastocyst (Wikipedia Commons)
Many fertility clinics and women who’ve had IVF treatment say that the transfer process is relatively painless. In all likelihood, your doctor won’t need to give you any medication. After you discuss your transfer, freezing, or discarding options, your doctor will perform the transfer and then you will be sent home to rest.
6. Testing for Pregnancy (14 days)
If all goes well, the embryo(s) will burrow deep into the uterine lining and become blastocysts. During this time, your clinic will prescribe progesterone to regulate your hormone levels. The body needs progesterone in order to help the uterine lining thicken and provide shelter for the fetus as it grows.
Fertility clinics allow 14 days to pass before testing for pregnancy using a blood test. If your pregnancy test is positive, the fertility clinic will usually continue to monitor your pregnancy until you begin to see an obstetrician.
For some, this is a time of celebration, but for others, sadness. Not all IVF procedures are successful. For example, an embryo can expire after the transfer process. Or, one or more transferred embryos or blastocysts may not implant.
Your clinic will provide you with a lot of information, and some things to look for during the 14 days after transfer.
Read more: IVF Pregnancy: 9 Very Important Things To Expect
There is no way to manipulate the body into becoming pregnant after the transfer phase. It will either happen or not. Also, there’s very little you can do to prevent it. The best thing to do is just to wait, and communicate any issues or questions you have with your fertility clinic.
IVF Procedures For Donor Eggs and Surrogates
The information above pertains to couples and single women using their own eggs and receiving an embryo transfer into their own bodies. However, for many couples, carrying a baby to term isn’t an option.
IVF for donor eggs and surrogates are similar, but different in just a few ways.
With donor eggs, the IVF procedures start at fertilization, really. So in those situations, a fertility doctor won’t be prescribing ovulation medication. However, suppression medication is still likely to be given, because embryo transfer has to take place at a certain point in your cycle.
Donor Egg IVF. In general, here are the high-level steps in the process:
- Fertility evaluation and assessment
- Pre-cycle preparation (may include suppression medication or other medication to improve the lining of your uterus).
- Sperm collection
- Fertilization
- Embryo transfer
- Testing for pregnancy
- Pregnancy
Most of the steps are the same, but the lengthy and sometimes challenging processes of inducing ovulation egg retrieval are not done in this case.
Surrogacy and IVF. The most common form of surrogate pregnancy happens through IVF. Either the surrogate receives the patient’s fertilized egg, her own, or a third (donor) egg. The IVF procedures are largely the same, unless a third (donor) egg is used instead of the surrogate woman’s or the intended mother’s egg.
When is Surrogate IVF used?
If a woman’s uterus has been removed but she still has functioning and healthy ovaries, a fertility doctor can collect her eggs, fertilize them, and then transfer the embryos or blastocysts to the surrogate mother. This is also true if carrying a baby to term is too dangerous for the mother.
Sometimes, couples or single women choose surrogate IVF using donor eggs. In these cases, none of the IVF procedures involve the intended mother, and only the later phases involve the surrogate mother. And in some cases, donor sperm may also be used.
Regardless of the IVF type – fresh or frozen eggs or sperm, donor eggs, or surrogacy, once the pregnancy occurs, the IVF process comes to a conclusion.
Conclusion
The IVF procedures and steps used in fertility treatment depend largely on the circumstances. In most cases, a woman and her spouse or partner both actively participate in all steps of the process. Sometimes, donor eggs and/or sperm are used, and other times, a surrogate mother will carry the baby for the parents. Once pregnancy takes place, the IVF process is complete, and will be considered successful. Congratulations! You can prepare to use our pregnancy calculator and hCG calculator to find out the due date and calculate beta hCG levels.